Sprained an ankle or a wrist? Touched something too hot? Caught a bug and have a fever? Overdid it and wound up with musculoskeletal pain?
The redness, swelling, heat, or pain you experience in these situations is your body’s inflammatory response to injury, irritant, or invasion.
Our immune response happens in response to a perceived irritant — it could be bacteria, maybe a trauma,exposure to toxins, or something like an injury or a burn.
Our immune system is built to deal with these irritants, identify and fight against harmful substances, and repair from injury and trauma.
This inflammatory response is your body’s immune system at work. It activates the body’s defenses and initiates healing responses and we need to ensure this process is working efficiently and effectively.
In this post, we’ll explore how to identify and maintain a healthy inflammatory response, as well as how to restore it to optimal function when it is unhealthy.

What is Acute Inflammation?
When we want water, we turn the faucet on. When we have the water we need, we turn it off. If we leave the water on, even just as a leak, it becomes wasteful, costly, and can lead to potential harm, such as flooding and mold formation.
Your body’s inflammatory response works in a similar way. It should ideally “turn on” when there is a need – this is known as acute inflammation.
However, as you address the underlying issue and heal, the inflammation should be turned off.
Common Inflammatory Responses
Often an “itis” (like hepatitis, dermatitis, etc) signals an inflammation that happens in that body space. Some of our inflammatory responses that are common include a fever that your body is producing when it’s fighting off an infection or a virus.
On the other hand, our immune system will trigger an inflammatory response to a bug bite if you’re bitten. Unfortunately, our immune system can sometimes go a bit haywire and begin to attack healthy cells and tissues in the body.
This is an autoimmune response and disease. Thus, addressing our inflammatory response (and what is triggering it) is part of management and healing of autoimmune conditions.
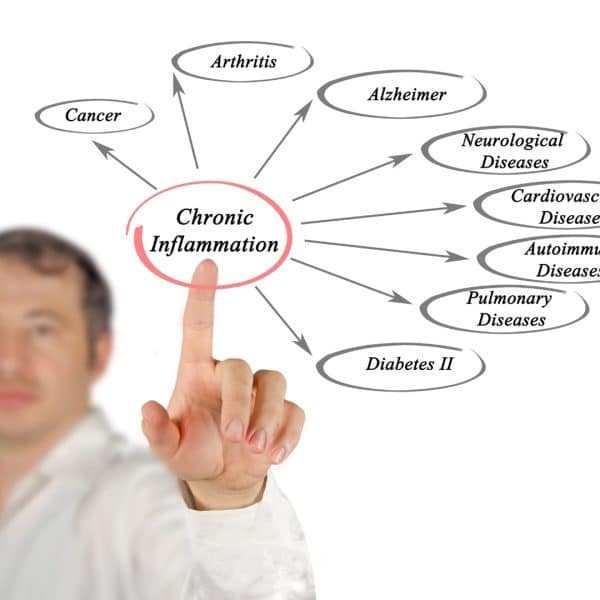
What is Chronic Inflammation?
If the inflammation persists even after your body has resolved the problem, it transforms into chronic inflammation – much like a leaky faucet.
Like a faucet, it should be turned on when needed but not left on as even the smallest drips can accumulate into something problematic over time. This is called “chronic inflammation”.
Detecting chronic inflammation can be more challenging, requiring an evaluation of symptoms and laboratory tests. Each person’s body is unique, so considering their genetics is crucial as well.
Chronic inflammation is linked to numerous diseases and can cause life-challenging symptoms. Therefore, it is of utmost importance to regularly monitor for signs of chronic inflammation to identify and address it as early as possible.
If we can prevent exposure to toxins or injury in the first place, that’s best. For example, can we avoid exposure to toxins in the environment or in our food etc. And in the same way, we can avoid injury and pain by working on proper exercise and balance.

Acute Inflammation Vs Chronic Inflammation: 11 Myths You Need To Know!
Myth #1: All Inflammation is Bad
Fact: Your body’s acute inflammatory response plays an important role in your overall health. It’s chronic inflammation that’s problematic.
Myth #2: Inflammation is Easy To Recognize
Fact: While acute inflammation often presents with noticeable symptoms like redness, swelling, and pain, chronic inflammation can be subtle and silent.
It may not manifest with typical signs, making it challenging to recognize without personalized evaluation.
Myth #3: Chronic Inflammation Only Affects Your Joints
Fact: Chronic inflammation can affect every system in the body and is thus a risk factor in all major diseases.
Myth #4: Inflammation Is Only Caused By An Infection
Fact: While acute inflammation is often a response to infection, chronic inflammation can arise from multiple factors.
Insufficient nutrient levels, ingredients that irritate your system, sedentary lifestyle, medications and surgeries, digestive dysfunction, chronic stress, and exposure to environmental toxins can all contribute to chronic inflammation, even in the absence of infection.
Myth #5: An Anti-inflammatory Diet Eliminates all Inflammation
Fact: As part of addressing chronic inflammation, following an anti-inflammatory diet personalized to your current needs today is an important part of your plan.
However, you may also need nutrient support to help repair and optimize nutrient levels that food and beverages can’t provide.
And like I mentioned in #5, your plan also needs to address your lifestyle choices — sleep, stress, activity etc. You may also need medication(s) or a protocol to address an infection, parasites etc.
Myth #6: Inflammation Can Be Cured With A Single Remedy
Fact: Chronic inflammation is a complex process influenced by several factors. Turning it “off” requires a multifaceted, personalized approach to ensure your body gets what it needs, and reduces exposure to irritants, while also doing any necessary repair work.
Myth #7: Increasing Your Omega-3’s Will turn Off Inflammation
Fact: Essential fatty acids including omega 3s and 6s play an important role in directing the inflammatory response.
While you may need to increase omega 3s from quality whole food sources (and possibly high-quality supplements), the body will respond favorably if you also reduce intake of poor-quality sources of fats.
Omega 6s have incorrectly been labeled “inflammatory” fats. In nature, foods are not omega 3 or omega 6 alone; in fact, your body needs essential omega 6s in a higher amount than omega 3s.
It’s when the body doesn’t have enough omega 3s and/or when the source of omega 6s are poor quality then they can cause trouble.
Myth #8: Carbs Cause Inflammation
Fact: Carbohydrates provide natural sugar, but they also deliver plant nutrients essential for a healthy inflammatory response.
Some carbohydrates — sweeteners, especially highly processed ones — do contribute to chronic inflammation. This is most likely to happen when they are consumed in excess and in the presence of digestive dysfunction.
Notably, non-nutritive sweeteners like Splenda® (sucralose), Equal® and NutraSweet® (aspartame), Sweet’N Low® (saccharin) and even natural ones like stevia alter the oral and digestive microbiome so they too can contribute to chronic inflammation.
Myth #9: More Protein Or Fats Are The Key To Turning Off Inflammation
Fact: Proteins and fats directly impact your inflammatory response. Thus, their quality and their quantity direct inflammation in a healthy or unhealthy direction.
Too much is never better. Likewise, choosing better quality proteins and fats in their whole food form is key.
For example, consuming the whole egg versus just the egg white or the whole bean/pea/nut versus a protein isolate or fat-free foods, as well as opting for food raised without ingredients that irritate the system.
Glyphosate-residue-free, certified organic, or raised without antibiotics are better choices to help you avoid irritants.
Animals (like us) produce inflammation when we are stressed or have poor digestion, so choosing animals raised and fed what they would experience more naturally helps reduce the inflammatory potential of their products.
Myth #10: Alcohol Reduces Inflammation
Fact: While the compounds in many foods that are turned into alcohol have anti-inflammatory benefits, the alcohol itself is still a toxin and can contribute to gut inflammation.
Depending on your genetics (for detoxification, inflammation, and oxidative stress) as well as your health goals, reducing or eliminating alcohol may be a benefit.
Myth #11: Over – The – Counter Painkillers Effectively Lower Chronic Inflammation
Fact: Over-the-counter pain medications like nonsteroidal antiinflammatory drugs (NSAIDs) can provide temporary relief from pain and inflammation.
However, they do not address the underlying “root” causes of chronic inflammation. Long-term reliance on painkillers without addressing lifestyle factors may mask symptoms while allowing inflammation to persist and potentially causing additional health problems.
Conclusion
Congratulations on reaching the end of our journey through the world of inflammation myths! By now, you’ve become well-versed in the crucial differences between acute inflammation and chronic inflammation. You’ve also discovered that inflammation isn’t as black-and-white as it’s often portrayed.
For example, as much as we might want it to be true, reaching for that drink won’t magically reduce inflammation. Alcohol may actually worsen inflammation, so moderation is key.
And don’t fall for the misconception that chronic inflammation only targets your joints. Oh no! Chronic inflammation can be a stealthy villain, affecting various parts of your body and contributing to a range of health issues.
Let’s not forget, not all carbs are guilty of causing inflammation. Whole grains, fruits, and veggies can be your allies in the battle against chronic inflammation.
Remember, not all inflammation is bad! Acute inflammation is your body’s superhero, protecting you from harmful invaders and initiating the healing process. It’s a natural response and a sign that your immune system is doing its job.
Now that you’ve separated fact from fiction, you can make informed choices to support your body’s natural defenses. Embrace a balanced lifestyle, rich in nutrient-packed foods, regular exercise, and stress management.
Want more tips on how to get rid of that nasty ole inflammation? Download my FREE e-book now and embark on a journey filled with easy-to-follow tips, and invaluable insights.
Discover how simple changes in your diet can make a world of difference in combating inflammation and promoting overall wellness.
In “The Power Of Plants To Fight Inflammation,” you’ll find a treasure trove of plant-based goodness, carefully curated to help you eat better and bid farewell to pesky inflammation. No more feeling held back by discomfort – it’s time to embrace a life full of vitality and energy!
Remember, it’s completely FREE, so there’s nothing to lose and everything to gain. Download your copy today and join the ranks of inflammation warriors armed with the Power of Plants! 💪🌱
***Disclaimer: This post is for informational purposes only and should not be construed as medical advice***


